Introduction
The coronavirus disease 2019 (COVID-19) is a respiratory and systemic disease that can infect multiple organs, including the lungs, heart, liver, and kidney. Transplantation is an established treatment for end-stage organ diseases, and patients commonly receive immunosuppressive therapy to prevent organ rejection Previous reports have conflicting results regarding if solid organ transplant recipients present an increased risk for COVID-19. Some reports suggest that immunosuppressive therapy reduces the severity of the COVID-19-associated inflammation, while other reports did not observe such an effect, reporting similar inflammation to non-SOT patients.
The SOT recipients may also respond differently to COVID-19 due to associated comorbidities, drugs used to prevent organ rejection, or the organ transplanted. Several case reports have investigated the COVID-19 outcome in solid organ transplant recipients. Nevertheless, no longitudinal comparison between different organ recipients has been made to this moment. In this article, a longitudinal investigation on COVID-19 course and survival analysis in SOT patients (recipients of heart, kidney, and liver) with over one and a half years post-transplant were analysed.
Heart and kidney transplant recipients presented an increase in several COVID-19 severity-associated biomarkers. Neutrophil-to-lymphocyte ratio and thrombocytopenia were higher in heart and kidney patients comparison to the control group and liver transplant recipients. Heart and kidney transplant recipients also presented an increase in the need for intensive care and invasive mechanical ventilation during the disease’s course. Importantly, heart and kidney transplant recipients presented a higher mortality rate in comparison to liver transplant recipients and non-transplant recipients. Further investigation involving immune response to SARS-CoV-2 in solid organ recipients should consider and separate patients according to the organ grafted.
Materials and Methods
In a cohort of 397 patients, 39 were solid organ transplant recipients: 25 kidney transplant recipients (Kidney), 7 heart transplant recipients (Heart), and 7 liver transplant recipients (Liver) (Table 1).
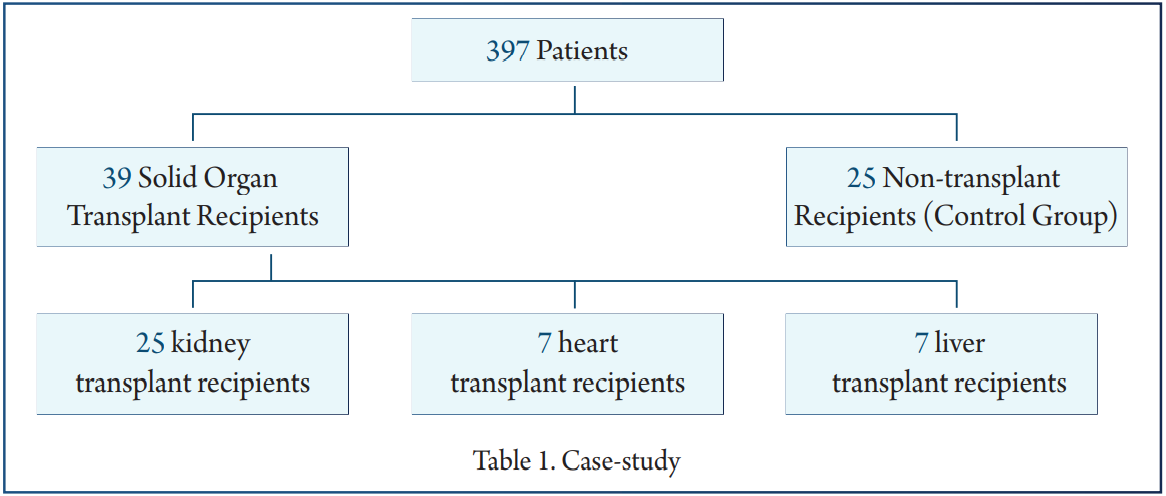
Exclusion criteria for all groups were the presence of other comorbidities except for systemic arterial hypertension (SAH) and type 1 & 2 diabetes mellitus (DM).
All patients with SAH underwent daily use of losartan (50 mg) for SAH control. Cyclosporine and tacrolimus levels on the serum were monitored and within the reference levels during COVID-19 (cyclosporine: 100–300 ng/mL and tacrolimus: 5–20 ng/mL). During hospitalization, COVID-19 patients received systemic and standard treatment. All patients received antibiotics (azithromycin) and anticoagulants. Part of the patients received antivirals (oseltamivir) and the other part received systemic corticosteroids (dexamethasone).
Statistical analyses were performed using the Kruskal–Wallis test with Dunn’s multiple comparisons and survival analyses were performed with the log-rank test for trend with GraphPad Prism-8 software.
All patients underwent solid organ transplants more than 18 months prior to SARS-CoV-2 infection. The control group consisted of 25 non-transplant recipients without comorbidities diagnosed with COVID-19 during the same period (Control).
Results
Most of the heart transplant patients (85.7%) required intensive care and invasive mechanical ventilation. This was also the outcome for 44% of the kidney transplant patients and 32% of the CONTROL group. This is in sharp contrast with the liver transplant recipients, none of whom evolved to this outcome. Neutrophil, lymphocyte counts, and the neutrophil-to-lymphocyte ratio (NTL) are considered COVID-19-associated severity biomarkers.
The percentage of patients with elevated NTL was significantly higher in the HEART and KIDNEY groups, especially the latter (86%). Additionally, noteworthy is the observation that none of the liver transplant recipients had abnormal NTL. We verified that the LIVER group presented a lower number of leukocytes during all hospitalization time compared with the three other groups.
Interestingly, renal function tests were abnormal in all patients of the three sot groups but in only a small fraction of the control (≤20%). This translated into a trend for higher urea and creatinine levels in the sot recipients, especially in the heart and kidney groups. Importantly, the survival analysis indicated a statistically better prognosis in the control and liver groups compared to the kidney and heart groups.
Conclusions
Our data indicate that heart and kidney recipient patients present an increase in COVID-19-associated inflammatory biomarkers during the disease course and lower survival rates in comparison to non-SOT patients and liver recipient patients. Further investigations should analyze the differential effects of COVID-19 in larger cohorts of specific organ transplant patients.
References
1. Dong, M.; Zhang, J.; Ma, X.; Tan, J.; Chen, L.; Liu, S.; Xin, Y.; Zhuang, L. ACE2, TMPRSS2 distribution and extrapulmonary organ injury in patients with COVID-19. Biomed. Pharmacother. 2020, 131, 110678.
2. Alberca, R.W.; Lima, J.C.; de Oliveira, E.A.; Gozzi-Silva, S.C.; Ramos, Y.Á.L.; de Souza Andrade, M.M.; Beserra, D.R.; de Mendonça Oliveira, L.; Branco, A.C.C.C.; Pietrobon, A.J.; et al. COVID-19 Disease Course in Former Smokers, Smokers and COPD Patients. Front. Physiol. 2021, 11, 637627.
3. Holman, N.; Knighton, P.; Kar, P.; O’Keefe, J.; Curley, M.; Weaver, A.; Barron, E.; Bakhai, C.; Khunti, K.; Wareham, N.J.; et al. Risk factors for COVID-19-related mortality in people with type 1 and type 2 diabetes in England: A population-based cohort study. Lancet Diabetes Endocrinol. 2020, 8, 823–833.
4. Zhang, H.; Dai, H.; Xie, X. Solid Organ Transplantation During the COVID-19 Pandemic. Front. Immunol. 2020, 11, 1392.
5. Zhu, L.; Xu, X.; Ma, K.; Yang, J.; Guan, H.; Chen, S.; Chen, Z.; Chen, G. Successful recovery of COVID-19 pneumonia in a renal transplant recipient with long-term immunosuppression. Am. J. Transplant. 2020, 20, 1859–1863.
6. Guillen, E.; Pineiro, G.J.; Revuelta, I.; Rodriguez, D.; Bodro, M.; Moreno, A.; Campistol, J.M.; Diekmann, F.; Ventura-Aguiar, P. Case report of COVID-19 in a kidney transplant recipient: Does immunosuppression alter the clinical presentation? Am. J. Transplant. 2020, 20, 1875–1878.
7. Azzi, Y.; Bartash, R.; Scalea, J.; Loarte-Campos, P.; Akalin, E. COVID-19 and Solid Organ Transplantation: A Review Article. Transplantation 2021, 105, 37–55.
8. Hage, R.; Steinack, C.; Benden, C.; Schuurmans, M.M. COVID-19 in Patients with Solid Organ Transplantation: A Systematic Review. Transplantology 2020, 1, 1–15.
9. Elias, M.; Pievani, D.; Randoux, C.; Louis, K.; Denis, B.; Delion, A.; Le Goff, O.; Antoine, C.; Greze, C.; Pillebout, E.; et al. COVID-19 infection in kidney transplant recipients: Disease incidence and clinical outcomes. J. Am. Soc. Nephrol. 2020, 31, 2413–2423.
10. Pereira, M.R.; Arcasoy, S.; Farr, M.A.; Mohan, S.; Emond, J.C.; Tsapepas, D.S.; Shi, Q.; Purpura, L.; Uhlemann, A.; Zucker, J.; et al. Outcomes of COVID-19 in solid organ transplant recipients: A matched cohort study. Transpl. Infect. Dis. 2021, e13637.
11. Ringer, M.; Azmy, V.; Kaman, K.; Tang, D.; Cheung, H.; Azar, M.M.; Price, C.; Malinis, M. A retrospective matched cohort single-center study evaluating outcomes of COVID-19 and the impact of immunomodulation on COVID-19-related cytokine release syndrome in solid organ transplant recipients. Transpl. Infect. Dis. 2021, 23, e13556.
12. Nacif, L.S.; Zanini, L.Y.; Waisberg, D.R.; Pinheiro, R.S.; Galvão, F.; Andraus, W.; D’albuquerque, L.C. COVID-19 in solid organ transplantation patients: A systematic review. Clinics 2020, 75, e1983.
13. Moosavi, S.A.; Mashhadiagha, A.; Motazedian, N.; Hashemazar, A.; Hoveidaei, A.H.; Bolignano, D. COVID-19 clinical manifestations and treatment strategies among solid-organ recipients: A systematic review of cases. Transpl. Infect. Dis. 2020, 22, e13427.
14. Trapani, S.; Masiero, L.; Puoti, F.; Rota, M.C.; Del Manso, M.; Lombardini, L.; Riccardo, F.; Amoroso, A.; Pezzotti, P.; Grossi, P.A.; et al. Incidence and outcome of SARS-CoV-2 infection on solid organ transplantation recipients: A nationwide population-based study. Am. J. Transplant. 2020, 21, 2509–2521.
15. Miarons, M.; Larrosa-García, M.; García-García, S.; Los-Arcos, I.; Moreso, F.; Berastegui, C.; Castells, L.; Pérez-Hoyos, S.; Varela, J.; Pau-Parra, A.; et al. COVID-19 in Solid Organ Transplantation: A Matched Retrospective Cohort Study and Evaluation of Immunosuppression Management. Transplantation 2021, 105, 138–150.
16. Mamode, N.; Ahmed, Z.; Jones, G.; Banga, N.; Motallebzadeh, R.; Tolley, H.; Marks, S.; Stojanovic, J.; Khurram, M.A.; Thuraisingham, R.; et al. Mortality Rates in Transplant Recipients and Transplantation Candidates in a High-prevalence COVID-19 Environment. Transplantation 2021, 105, 212–215.
17. Avery, R.K.; Chiang, T.P.Y.; Marr, K.A.; Brennan, D.C.; Sait, A.S.; Garibaldi, B.T.; Shah, P.; Ostrander, D.; Steinke, S.M.; Permpalung, N.; et al. Inpatient COVID-19 outcomes in solid organ transplant recipients compared to non-solid organ transplant patients: A retrospective cohort. Am. J. Transplant. 2020, 21, 2498–2508.





